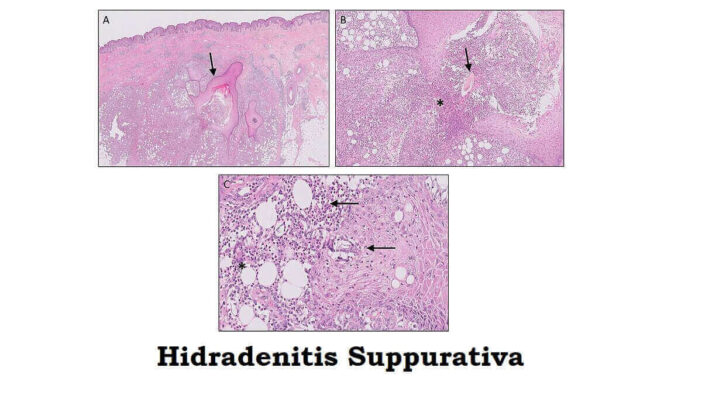
Healthbeautyidea.com – Hidradenitis Suppurativa is a disease characterized by the onset of small lumps the size of nuts under the skin. Lumps can be painful and pus-filled. This condition is often referred to as acne inversa.
Hidradenitis Suppurativa arises on skin that has hair and sweat glands, especially in areas that often experience friction, such as the armpits, groin, thigh folding, buttocks, and breasts. This condition tends to occur after puberty and lasts for a long period of time (chronic).
In severe cases, pus ducts can form under the skin, otherwise known as pilonidal sinus. The duct is connected with many lumps, so infection and inflammation can spread to other areas.
Hidradenitis Suppurativa Symptoms
Some of the symptoms of Hidradenitis Suppurativa include:
- Common in the armpits, thigh folds, and perianal.
- Lumps with pus on the skin (0.5-2 centimeters).
- Signs of inflammation of the affected skin, such as redness and feeling warm.
- Multiple abscesses, fistulas, and sinuses can form, in chronic inflammation.
Hidradenitis Suppurativa Causes
Hidradenitis Suppurativa until now has not been known the exact cause. The disease can occur in all limbs with hair follicles, which are initially triggered by the presence of hair follicle blockages and then inflames.
Hidradenitis Suppurativa Risk Factors
Some risk factors for Hidradenitis Suppurativa include:
- Age, which generally occurs during puberty, is around the age of 20 to 29 years.
- Genetics, which is experienced if it has a history of this disease in the family, but is not associated with poor hygiene.
- Gender, i.e. Women are more likely to develop this disease than men.
- Smo**king habit.
- Obesity.
- Diabetes.
- Metabolic syndrome.
- Crohn’s disease.
Hidradenitis Suppurativa Diagnosis
Determination of the diagnosis of suppurative Hidradenitis skin disease is enough to be done through physical examination of the affected area. The patient may show the presence of painful lumps and accompanied by an abscess, the presence of the sinuses in the axillary, groin or perineum areas.
Hidradenitis Suppurativa is often mistaken for acne or folliculitis (inflammation of the hair follicles). To confirm the diagnosis, the doctor will perform the following tests:
Q&A
The doctor will ask about the patient’s history of illness, signs and symptoms, and risk factors.
Physical examination of the skin
The doctor will perform a physical examination by examining the affected area of the skin.
Laboratory tests
No laboratory examination can diagnose this condition. However, the doctor can take a swab from the infected part or take a sample of pus and fluid coming out of the lesion.
The samples were then examined in a laboratory to rule out other skin infections.
Hidradenitis Suppurativa Stages
Based on the severity of the disease, Hidradenitis Suppurativa is classified into three stages according to Hurley’s stage, namely:
- Stage one is a solitary or multi-threaded abscess that is firmly bordered, without scars and without sinus ducts.
- The second stage is the formation of a recurrent abscess, with the formation of the sinus tract.
- The third stage indicates fused abscess lesions, scarring, and the fused of the sinus tract.
Complications of Hidradenitis Suppurativa
If the lump does not improve and recurs frequently, the patient is likely to experience the following complications.
Scar
Lumps on the skin are at risk of rupture and leaving scars. The scars that arise can thicken and take a long time to disappear.
Infection
The area of the lump that is ruptured and injured can be infected.
Can’t move freely
Lumps and wounds on the skin will hurt and cause you difficulty moving parts of the body freely.
Skin discoloration
Certain areas of your skin, especially those with bumps, will turn darker.
Depression
The appearance of skin full of bumps, wounds, and odors can decrease confidence. This can result in the patient feeling sad, even depressed.
Lymph blockage
Lumps and scars on the surface of the skin may be located around the lymph nodes. This can affect the flow of lymph fluid, which can cause swelling.
Skin Cancer
Although very rare, Hidradenitis Suppurativa has the possibility of triggering the appearance of skin cancer.
Source:
- Image: Jenny Giang, Marc A. J. Seelen, Martijn B. A. van Doorn, Robert Rissmann,Errol P. Prens and Jeffrey Damman, CC BY 4.0 https://creativecommons.org/licenses/by/4.0, via Wikimedia Commons





 Skincare Solutions & Skin Health
Skincare Solutions & Skin Health
 Mental Health, Stress & Emotional Wellbeing
Mental Health, Stress & Emotional Wellbeing Sleep, Energy & Daily Performance
Sleep, Energy & Daily Performance